Medical Chatbot: Guide 2026

Medical Chatbot: Guide 2026
In 2026, the healthcare system operates under the pressure of staff shortages, a growing number of patients, and the ongoing digitization of processes. In this context, a medical chatbot is no longer a technological curiosity but an operational tool. At the same time, the market has become saturated with solutions of highly varying quality – from simple informational assistants to systems supporting clinical decision-making. The differences between them concern the scope of responsibility. As a result, the term “medical chatbot” today encompasses both low-risk tools and systems potentially subject to medical device regulations.
This guide organizes definitions, categories of use, and implementation requirements. Its objective is to provide evaluation criteria – technological, organizational, and regulatory – that enable informed and measurable decision-making.
What is a medical chatbot?
A medical chatbot is an intelligent online assistant that helps patients obtain necessary health information more quickly. The key functions of a chatbot include:
- answering questions about symptoms,
- providing guidance on whether a medical consultation is advisable,
- reminding patients about medications,
- assisting with appointment scheduling.
This technology operates within mobile applications, clinic websites, or telemedicine systems. It does not replace a physician but supports both patients and medical staff in daily tasks. Thanks to artificial intelligence, it can conduct natural conversations and tailor responses to the user’s situation. In 2026, medical chatbots are becoming increasingly advanced and are genuinely relieving pressure on healthcare systems.
Technological foundations of a medical chatbot in 2026
A modern medical chatbot is no longer a simple rule-based system built on decision trees. Its operation is based on advanced large language models (LLMs) capable of analyzing conversational context, understanding linguistic nuances, and generating responses resembling natural dialogue. These models are trained on large datasets and, in medical applications, additionally fine-tuned using verified clinical sources.
A key technological element is integration with medical systems such as EHR/EMR. This allows the chatbot, within controlled parameters, to access a patient’s medical history, test results, or information about prescribed medications. In practice, this enables more personalized and accurate responses. Interoperability standards such as HL7 and FHIR facilitate secure data exchange between different healthcare systems.
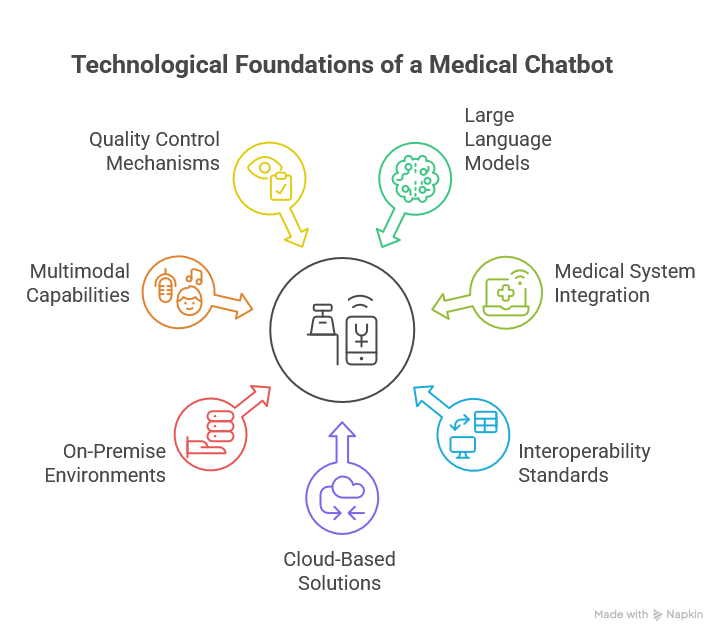
Implementation architecture is also crucial. Cloud-based solutions provide scalability and rapid model updates, while on-premise environments offer greater control over sensitive data. The choice depends on regulatory requirements, security policies, and the organization’s budget.
Modern chatbots are increasingly multimodal. This means they can analyze not only text but also speech (speech recognition and synthesis) and images, such as photographs of skin lesions. Combined with quality control mechanisms, content filtering, and clinical risk monitoring, this creates a coherent technological ecosystem.
The technological foundation of a medical chatbot is therefore not a single algorithm but a complex infrastructure combining artificial intelligence, system integrations, data security, and quality assurance mechanisms.
Types of medical chatbots
Medical chatbots do not constitute a uniform technological category but include diverse solutions designed for specific clinical and operational objectives. Their classification depends on the scope of system responsibility, regulatory risk level, and the degree of integration with a medical facility’s IT infrastructure. Understanding these types is essential for selecting the appropriate technology.
Triage chatbots (initial patient qualification)
Triage chatbots are used for preliminary assessment of symptoms reported by patients. Based on structured questions, the system analyzes reported symptoms and determines urgency levels: from self-care, through consultation with a primary care physician, to immediate medical intervention. They do not provide diagnoses but support the decision-making process and help reduce pressure on call centers and emergency departments. The effectiveness of such systems depends on algorithm quality, up-to-date clinical knowledge, and properly designed safety pathways.
Patient assistants and monitoring
This type of chatbot focuses on long-term patient support. They may remind patients about medication intake, follow-up appointments, or required tests. In the case of chronic diseases (e.g., diabetes or hypertension), they support monitoring of health parameters and respond to concerning values. WHO epidemiological data indicate that chronic diseases account for more than 70% of the global disease burden, and proper monitoring and support can reduce the risk of complications by up to 30%. These systems often integrate with wearable devices, enabling automated data collection and more personalized support.
Administrative chatbots
Administrative solutions automate organizational processes such as:
- appointment scheduling,
- form completion,
- providing information about opening hours,
- preparation instructions for medical tests,
- handling e-referrals and e-prescriptions,
- managing appointment cancellation and rescheduling processes.
Their primary objective is to reduce operational costs and shorten patient service time. In practice, they are the most commonly implemented type of chatbot in medical facilities. Market analyses indicate that up to 68% of AI implementations in healthcare concern administrative or patient service support solutions. Additionally, they enable standardized patient communication, reducing the risk of misinformation and ambiguous instructions. When integrated with HIS systems, they can automatically update appointment statuses, send SMS/email notifications, and synchronize data with medical staff calendars.
Porozmawiaj z naszym specjalistą
Clinical and therapeutic support
Some chatbots support medical personnel in document analysis or assist patients in the mental health domain by offering structured therapeutic conversations. These require particularly rigorous validation and a clearly defined boundary of system responsibility.
Practical benefits of chatbot implementation – how can it help?
The decision to implement a medical chatbot concerns not only technology but also the overall functioning of the facility. Such a system affects information flow, work organization, and the patient service model. Its real value can only be assessed through analysis of specific process improvements and their impact on operational outcomes.
Relieving operational processes
The implementation of a medical chatbot brings measurable operational, financial, and organizational benefits. The most immediate effect is reducing the burden on reception desks and call centers. The system handles repetitive inquiries regarding opening hours, specialist availability, preparation for tests, or appointment status. This allows staff to focus on tasks requiring genuine interaction and decision-making.
Increasing accessibility and continuity of service
Another significant advantage is improved service accessibility. A chatbot operates 24/7, regardless of the facility’s working hours. According to the US Healthcare Consumer Survey, 40–50% of patients have used telemedicine and expect it to remain a permanent element of healthcare services. Patients can schedule appointments, reschedule visits, or obtain basic information without waiting in a phone queue. This shortens service time and reduces missed calls, which often translate into lost revenue.
Supporting clinical processes
In the clinical domain, a chatbot can assist with preliminary patient qualification. A structured pre-visit interview enables collection of key information before consultation, shortening visit duration and increasing its efficiency. In chronic care management, the system can provide medication and follow-up reminders, reducing the risk of therapy interruptions.
Cost reduction and management support
An important aspect is the reduction of operational costs. Automation of administrative processes reduces demand for human resources in low value-added areas. At the same time, the chatbot generates analytical data: most common questions, peak load hours, or reasons for appointment cancellations. This information supports facility management and process optimization.
Standardization, improved customer experience, and scalability
Additionally, implementing such a solution strengthens the image of a modern organization, increases patient satisfaction, and improves communication standardization. As a result, the chatbot becomes not only a technological tool but also an element of the strategy for the development and scaling of medical services.
![]()
The implementation process of a medical chatbot in a healthcare facility
The implementation of a medical chatbot is a multi-stage process. Due to the processing of sensitive data and the potential impact on clinical decisions, implementation requires formal risk analysis and close cooperation between IT departments, medical staff, and legal teams. For better clarity, the stages of this implementation are presented below:
- Needs analysis and functional scope definition
The process begins with identifying the business or clinical problem. It must be determined whether the chatbot is to support registration, triage, patient monitoring, or medical staff. The target group, user volume, and measurable objectives (e.g., 30% reduction in service time) are defined. A preliminary risk analysis is also conducted at this stage. - Regulatory and legal assessment
The next step is determining whether the solution qualifies as a medical device under MDR or other regulations. Compliance with GDPR, sensitive data processing rules, and patient consent requirements are analyzed. If necessary, compliance documentation and audit procedures are prepared. - Architecture design and IT integration
At this stage, the technical architecture is defined: cloud or on-premise, authentication methods, and integration with HIS/EHR systems. Ensuring secure data transmission and access control becomes critical. - Configuration, testing, and clinical validation
The system is then adapted to facility procedures. Functional and security tests are conducted, and in clinical applications, substantive validation with medical staff participation. Response effectiveness, information completeness, and error scenarios are assessed. - Staff training and pilot launch
Before full implementation, a pilot is conducted within a selected organizational unit. Staff receive training regarding system scope and escalation procedures. According to McKinsey’s report “Unlocking Success in Digital Transformations,” projects in which organizations invest in training and active change management are more than 2.5 times more likely to achieve their intended objectives. - Monitoring, optimization, and continuous oversight
After launch, the system is subject to continuous monitoring. Efficiency indicators, user reports, and security incidents are analyzed. The model should be periodically updated, and procedures adjusted to regulatory and organizational changes.
Funding for healthcare facilities – what sources support chatbot investments?
In 2026, the healthcare sector still have access to numerous support instruments enabling the modernization of digital infrastructure and the implementation of AI-based solutions. However, WHO research indicates that only 8% of countries have national AI strategies in healthcare, indirectly reflecting the early organizational stage of many implementations. Facilities planning investments in chatbots, medical voicebots, patient service automation systems, or analytical tools can use several key national and EU programs.
- The National Recovery Plan (KPO) – particularly components D1.1.2 and D1.2.1 – focuses on healthcare digitization, medical data analysis, and cybersecurity enhancement. Projects involving chatbot solutions align with these objectives as part of e-health development and patient communication improvement.
- The FENiKS Program (European Funds for Infrastructure, Climate, Environment) provides support for larger healthcare entities. Funding may include the purchase of modern equipment and the development of IT systems supporting management and medical processes.
- Regional Operational Programs (RPO) at the voivodeship level enable funding of innovative projects, including within the SME sector. They represent a viable option for private clinics and smaller medical centers planning digitization.
- The Medical Fund, including the Subfund for Modernization of Healthcare Entities, provides resources dedicated to digital security development and modernization of diagnostic infrastructure.
- Additionally, the SMART Path under FENG and grants from NCBR enable funding of research and development projects, particularly in collaboration with scientific institutions.
A detailed analysis of available support instruments for AI projects in healthcare is presented in our dedicated study: AI in medicine 2026: 5 real funding sources your facility can use.
AI in healthcare: implement wisely or not at all
In 2026, a medical chatbot is an operational tool, not a marketing one. Its value is measured by three parameters:
- reduction of staff workload,
- shortened access time to information and services,
- control of clinical, legal, and reputational risk.
Solutions that do not integrate with medical systems, lack a clear accountability model, and are not based on current clinical guidelines should not be implemented. AI in healthcare makes sense only when it improves efficiency.
In 2026, the question is not “whether to implement medical chatbots?” but “how to implement them so that they genuinely improve operational outcomes and quality of care?”
EasyCall designs and implements systems tailored to real processes within healthcare facilities. We support organizations not only in needs analysis and technology implementation but also in obtaining information about available funding opportunities, including national and EU programs. As a result, implementation is not only cost-optimized but also carried out efficiently. Cooperation with EasyCall means a project-based approach, clearly defined objectives, and ready-to-use solutions.
